Paper:
Evaluation of Muscle Activity and Human Standing Stability Index Using the Swash Plate in a Disturbance Application
Tsutomu Togoe*, Pham Hoang Tung*, Koki Honda**, Yasutaka Nakashima**, and Motoji Yamamoto**
*Department of Mechanical Engineering, Graduate School of Engineering, Kyushu University
744 Motooka, Nishi-ku, Fukuoka, Fukuoka 819-0395, Japan
**Department of Mechanical Engineering, Faculty of Engineering, Kyushu University
744 Motooka, Nishi-ku, Fukuoka, Fukuoka 819-0395, Japan
Human standing stability was evaluated using a swash plate drop device in a disturbance application. Under different experimental conditions using the device, electromyogram (EMG) measurements showed that the left and right lower limb muscles were used differently. It also demonstrated that the dynamics also differed depending on the experimental conditions. In particular, the dynamics of standing stabilization in a tandem standing position and a normal standing position significantly differed, and the activities of related muscles were also significantly different; this indicates that standing stability may potentially depend on the subjects. These results indicate the need for the comprehensive consideration of the standing and disturbance conditions during the quantitative evaluation of human standing stability.
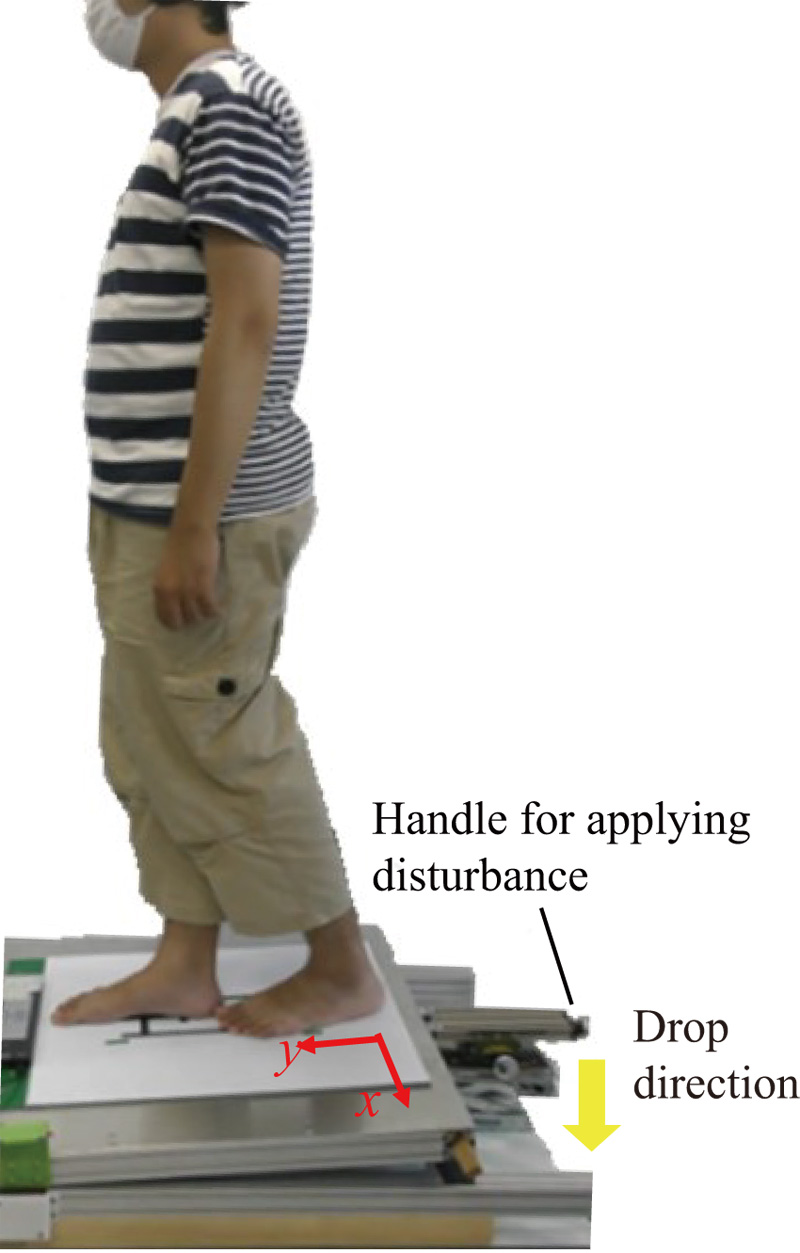
Human standing stability evaluated using a swash plate drop device
- [1] T. Furuna and H. Shimada, “Gait and falls in elderly people – Epidemiological Study,” J. of the Society of Biomechanisms, Vol.30, No.3, pp. 132-137, 2006.
- [2] L. Z. Rubenstein, “Falls in older people epidemiology, risk factors and strategies for prevention,” Age and Ageing, Vol.35, No.2, pp. 37-41, 2006.
- [3] H. C. Diener, J. Dichgans, F. Booz, and M. Bacher, “Early stabilization of human posture after a sudden disturbance influence of rate and amplitude of displacement,” Experimental Brain Research, Vol.56, No.1, pp. 126-134, 1984.
- [4] S. Tsuji and J. Miyazaki, “Characteristics of Mental and Physical Functions Related to Lateral Falls among Community-dwelling Elderly Individuals,” Rigakuryoho Kagaku, Vol.34, No.4, pp. 405-410, 2019 (in Japanese).
- [5] M. Kobayashi and Y. Shimizu, “Effect of Foot Insole on Standing Balance,” Rigakuryoho Kagaku, Vol.29, No.4, pp. 605-607, 2014 (in Japanese).
- [6] M. Ishida and K. Sagawa, “Quantative Evaluation for Standing Stability during Anterior-Posterior Body Tilt Movement Using Inverted Pendulum Model,” Trans. of the Japan Society of Mechanical Engineers, Series C, Vol.75, No.752, pp. 1047-1055, 2009.
- [7] T. Hiramatsu and K. Izumi, “Relationship between characteristics of plantar pressure distribution while standing and falls in community-dwelling elderly,” J. of the Tsuruma Health Science Society Kanazawa University, Vol.34, No.2. pp. 51-63, 2011.
- [8] A. L. Hof, M. G. J. Gazendam, and W. E. Sinke, “The condition for dynamic stability,” J. of Biomechanics, Vol.38, No.1, pp. 1-8, 2005.
- [9] N. Nawayseh and M. J. Griffin, “Effect of frequency, magnitude and direction of translational and rotational oscillation on the postural stability of standing people,” J. of Sound and Vibration, Vol.298, No.3, pp. 725-754, 2006.
- [10] A. D. Kuo, “An optimal state estimation model of sensory integration in human postural balance,” J. of Neural Engineering, Vol.2, No.3, pp. S235-S249, 2005.
- [11] P. Hur, B. A. Duiser, S. M. Salapaka, and E. T. H. Wecksler, “Measuring robustness of the postural control system to a mild impulsive perturbation,” IEEE Trans. on Neural Systems and Rehabilitation Engineering, Vol.18, No.4, pp. 461-467, 2010.
- [12] Y. Nakashima, T. Matsuo, P. H. Tung, T. Togoe, and M. Yamamoto, “The Evaluation Method of Standing Stability by Applying the Disturbance of Swash Plate Fall,” Proc. of the 24th Robotics Symposia, Vol.1, No.D4, pp. 47-52, 2019.
- [13] S. M. Henry, J. Fung, and F. B. Horak, “Control of stance during lateral and anterior/posterior surface translations,” IEEE Trans. on Rehabilitation Engineering, Vol.6, No.1, pp. 32-42, 1998.
- [14] F. C. Kuo, C. Z. Hong, C. L. Lai, and S. H. Tan, “Postural control strategies related to anticipatory perturbation and quick perturbation in adolescent idiopathic scoliosis,” Spine, Vol.36, No.10, pp. 810-816, 2011.
- [15] E. T. H. Wecksler, K. Katdare, J. Matson, W. Liu, L. A. Lipsitz, and J. J. Collins, “Predicting the dynamic postural control response from quiet-stance behavior in elderly adults,” J. of Biomechanics, Vol.36, No.9, pp. 1327-1333, 2003.
- [16] T. Buchanan, D. G. Lloyd, K. Manal, and T. Besier, “Estimation of muscle forces and joint moments using a forward-inverse dynamics model,” Medicine and Science in Sports and Exercise, Vol.37, No.11, pp. 1911-1916, 2005.
- [17] S. Sozzi, J. L. Honeine, M. C. Do, and M. Schieppati, “Leg muscle activity during tandem stance and the control of body balance in the frontal plane,” Clinical Neurophysiology, Vol.124, No.6, pp. 1175-1186, 2013.
 This article is published under a Creative Commons Attribution-NoDerivatives 4.0 Internationa License.
This article is published under a Creative Commons Attribution-NoDerivatives 4.0 Internationa License.