Paper:
Classification of Care Assistive Technology Based on the Relationship Between Users and Technologies
Hiroyasu Miwa*, Kentaro Watanabe*, and Marketta Niemelä**
*National Institute of Advanced Industrial Science and Technology (AIST)
6-2-3 Kashiwanoha, Kashiwa, Chiba 277-0882, Japan
**VTT Technology Research Centre of Finland Ltd.
Visiokatu 4, Tampere / P.O. Box 1300, Tampere 33101, Finland
While an aging population in Japan and other countries is resulting in an increased demand for nursing care services, there is a shortage of care workers due to a decrease in the working population. The use of care assistive technologies such as robots, artificial intelligence, and information technology is expected to compensate for this shortage, and many care assistive technologies such as power assist devices and communication robots have been developed. However, their introduction and widespread use in actual service have not progressed. The aim of this study is to address the problem on less technology introduction in nursing care by surveying the attitudes of potential users to care assistive technologies, clarify the factors affecting the use of such technologies, and propose a new design method for the technologies. We surveyed attitudes to the use of care assistive technology from the perspective of function and information utilization for three groups: active seniors, informal carers, and formal carers. The survey was conducted in Japan and Finland, which have high aging populations. Based on the survey results, we proposed, as a design method, a classification of care assistive technologies according to their interaction with users as well as the nursing care process.
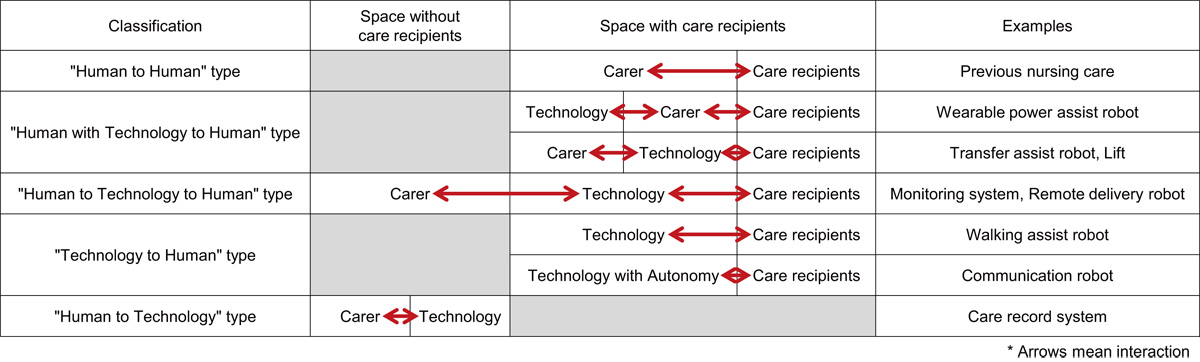
Classification of care assistive technology
- [1] Cabinet Office, “Annual Report on the Aging Society in 2018,” Nikkei Printing Inc., pp. 2-3, 2018.
- [2] National Institute of Population and Social Security Research, “Population Projections for Japan (2017): 2016 to 2065,” p. 3, p. 19, p. 24, 2017.
- [3] K. Coco, M. Kangasniemi, and T. Rantanen, “Care Personnel’s Attitudes and Fears Toward Care Robots in Elderly Care: A Comparison of Data from the Care Personnel in Finland and Japan,” J. of Nursing Scholarship, Vol.50, No.6, pp. 624-644, doi: 10.1111/jnu.12435, 2018.
- [4] K. Miura, H. Kadone, M. Koda, T. Abe, H. Kumagai, K. Nagashima, K. Mataki, K. Fujii, H. Noguchi, T. Funayama, H. Kawamoto, Y. Sankai, and M. Yamazaki, “The hybrid assistive limb (HAL) for Care Support successfully reduced lumbar load in repetitive lifting movements,” J. of Clinical Neuroscience, Vol.53, pp. 276-279, doi: 10.1016/j.jocn.2018.04.057, 2018.
- [5] K. Miura, H. Kadone, T. Abe, M. Koda, T. Funayama, H. Noguchi, H. Kumagai, K. Nagashima, K. Mataki, Y. Shibao, K. Sato, H. Kawamoto, Y. Sankai, and M. Yamazaki, “Successful Use of the Hybrid Assistive Limb for Care Support to Reduce Lumbar Load in a Simulated Patient Transfer,” Asian Spine J., Vol.15, No.1, pp. 40-45, doi: 10.31616/asj.2019.0111, 2021.
- [6] Y. Satoh, T. Yamada, Y. Arai, R. Shimamura, M. Hirosawa, R. Yamakawa, and S. Takagi, “The immediate effect of the Honda Walking Assist Device on foot and ankle function in hemiplegic stroke patients,” The J. of Physical Therapy Science, Vol.32, pp. 405-409, doi: 10.1589/jpts.32.405, 2020.
- [7] T. G. Stavropoulos, A. Papastergiou, L. Mpaltadoros, S. Nikolopoulos, and I. Kompatsiaris, “IoT Wearable Sensors and Devices in Elderly Care: A Literature Review,” Sensors, Vol.20, Issue 10, 2826, doi: 10.3390/s20102826, 2020.
- [8] K. Wada, Y. Takasawa, and T. Shibata, “Robot therapy at facilities for the elderly in Kanagawa prefecture – a report on the experimental result of the first month,” Proc. of the 23rd IEEE Int. Symp. on Robot and Human Interactive Communication, pp. 193-198, 2014.
- [9] G. W. Lane, D. Noronha, A. Rivera, K. Craig, C. Yee, B. Mills, and E. Villanueva, “Effectiveness of a social robot, “Paro,” in a VA long-term care setting,” Psychological Services, Vol.13, No.3, pp. 292-299, doi: 10.1037/ser0000080, 2016.
- [10] M. Kawakami, S. Toba, K. Fukuda, S. Hori, Y. Abe, and K. Ozaki, “Application of Deep Learning to Develop a Safety Confirmation System for the Elderly in a Nursing Home,” J. Robot. Mechatron., Vol.29, No.2, pp. 338-345, doi: 10.20965/jrm.2017.p0338, 2017.
- [11] K. Wada, T. Shibata, T. Asada, and T Musha, “Robot Therapy for Prevention of Dementia at Home – Results of Preliminary Experiment,” J. Robot. Mechatron., Vol.19, No.6, pp. 691-697, doi: 10.20965/jrm.2007.p0691, 2007.
- [12] T. Shibata and J. F. Coughlin, “Trends of Robot Therapy with Neurological Therapeutic Seal Robot, PARO,” J. Robot. Mechatron., Vol.26, No.4, pp. 418-425, doi: 10.20965/jrm.2014.p0418, 2014.
- [13] Yano Research Institute Ltd., “Market of ICT for the Aged/Long Term Care 2016,” p. 50, 2016 (in Japanese).
- [14] H. Miwa, T. Fukuhara, and T. Nishimura, “Service process visualization in nursing-care service using state transition model,” J. C. Spohrer and L. E. Freund (Eds.), “Advances in the Human Side of Service Engineering,” Springer, pp. 3-12, 2012.
- [15] H. Miwa, K. Watanabe, T. Fukuhara, T. Nagao, and T. Nishimura, “Proposal of Quality Study for Nursing-Care Service,” L. Freund and W. Cellary (Eds.), “Advances in the Human Side of Service Engineering,” Springer, pp. 442-449, 2014.
- [16] H. Miwa and K. Watanabe, “Toward Service Process Improvement in Nursing-Care Services – Application of Behavior Measurement –,” T. Takenaka, H. S. Han, and C. Minami (Eds.), “Serviceology for Services,” Springer, pp. 253-265, 2020.
- [17] K. Watanabe and M. Niemelä, “Aging and technology in Japan and Finland – Comparative remarks,” M. Toivonen and E. Saari (Eds.), “Human-Centered Digitalization and Services,” Springer, pp. 155-175, 2019.
- [18] H. Miwa, K. Watanabe, M. Ylikauppila, M. Kulju, and M. Niemelä, “Time and Motion Study of Nursing-Care Services in Japan and Finland,” Proc. of ICSSI2018 and ICServ2018, pp. 144-147, 2018.
- [19] K. Watanabe and K. Fukuda, “Designing Digital Technology for Service Work: Systematic and Participatory Approach,” Proc. of the 22nd Int. Conf. on Engineering Design (ICED19), pp. 5-8, 2019.
- [20] A. De Keyser, S. Köcher, L. Alkire (née Nasr), C. Verbeeck, and J. Kandampully, “Frontline Service Technology infusion: conceptual archetypes and future research directions,” J. Serv. Manage, Vol.30, No.1, pp. 156-183, doi: 10.1108/JOSM-03-2018-0082, 2019.
- [21] P. Rantanen, T. Parkkari, S. Leikola, M. Airaksinen, and A. Lyles, “An In-home Advanced Robotic System to Manage Elderly Home-care Patients’ Medications: A Pilot Safety and Usability Study,” Clinical Therapeutics, Vol.39, Issue 5, pp. 1054-1061, doi: 10.1016/j.clinthera.2017.03.020, 2017.
 This article is published under a Creative Commons Attribution-NoDerivatives 4.0 Internationa License.
This article is published under a Creative Commons Attribution-NoDerivatives 4.0 Internationa License.