Research Paper:
Non-Contact Sleep Stage Estimation by Updating its Prediction Probabilities According to Ultradian Rhythm
Iko Nakari
 and Keiki Takadama
and Keiki Takadama

The University of Electro-Communications
1-5-1 Chofugaoka, Chofu, Tokyo 182-8585, Japan
To increase an accuracy of the sleep stage estimation without connecting any devices/electrodes to the body, this paper proposes the updating method for its estimation according to an ultradian rhythm as one of the biological rhythms of humans. In the proposed method, the prediction probability of the sleep stage is updated by the Widrow–Hoff learning rule which is generally employed in the update of reinforcement learning. Through the human subject experiment which acquired the biological vibration data from the mattress sensor during sleep, the following implications have been revealed: (1) the accuracy and the quadratic weighted kappa (QWK) of the sleep stage estimation updated by the proposed method are higher than those of random forest (RF) as the conventional method; (2) the multiple update of the probability of the sleep stage according to the ultradian rhythm is significantly important to improve its accuracy and QWK; and (3) compared with RF which over-estimated the NR2 stage while less-estimated the NR1 and NR3 stages, the proposed method contributes to correctly estimating the NR1–3 stages thank to the follow of the ultradian rhythm.
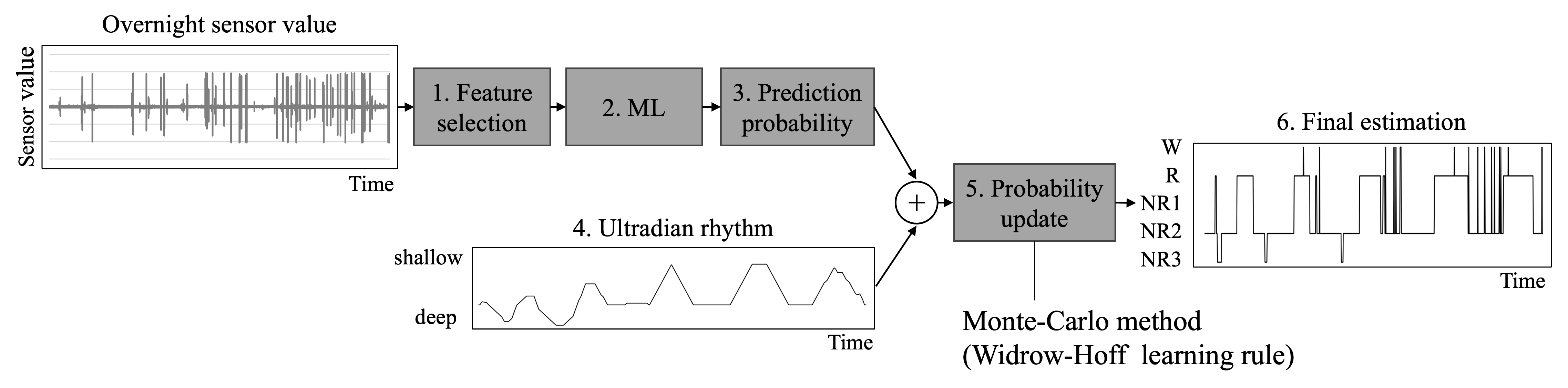
Update estimation with the Monte-Carlo method
- [1] J. M. Mullington, M. Haack, M. Toth, J. M. Serrador, and H. K. Meier-Ewert, “Cardiovascular, inflammatory, and metabolic consequences of sleep deprivation,” Progress in Cardiovascular Diseases, Vol.51, No.4, pp. 294-302, 2009. https://doi.org/10.1016/j.pcad.2008.10.003
- [2] C. Holingue, A. Wennberg, S. Berger, V. Y. Polotsky, and A. P. Spira, “Disturbed sleep and diabetes: A potential nexus of dementia risk,” Metabolism, Vol.84, pp. 85-93, 2018. https://doi.org/10.1016/j.metabol.2018.01.021
- [3] A. Q. Javaid, C. M. Noble, R. Rosenberg, and M. A. Weitnauer, “Towards sleep apnea screening with an under-the-mattress IR-UWB radar using machine learning,” 2015 IEEE 14th Int. Conf. on Machine Learning and Applications (ICMLA), pp. 837-842, 2015. https://doi.org/10.1109/ICMLA.2015.79
- [4] A. Tal, Z. Shinar, D. Shaki, S. Codish, and A. Goldbart, “Validation of contact-free sleep monitoring device with comparison to polysomnography,” J. of Clinical Sleep Medicine, Vol.13, No.3, pp. 517-522, 2017. https://doi.org/10.5664/jcsm.6514
- [5] H. Scott, L. Lack, and N. Lovato, “A pilot study of a novel smartphone application for the estimation of sleep onset,” J. of Sleep Research, Vol.27, No.1, pp. 90-97, 2018. https://doi.org/10.1111/jsr.12575
- [6] H. Hong, L. Zhang, H. Zhao, H. Chu, C. Gu, M. Brown, X. Zhu, and C. Li, “Microwave sensing and sleep: Noncontact sleep-monitoring technology with microwave biomedical radar,” IEEE Microwave Magazine, Vol.20, No.8, pp. 18-29, 2019. https://doi.org/10.1109/MMM.2019.2915469
- [7] J. Liu, Y. Zhao, B. Lai, H. Wang, and K. L. Tsui, “Wearable device heart rate and activity data in an unsupervised approach to personalized sleep monitoring: algorithm validation,” JMIR Mhealth and Uhealth, Vol.8, No.8, Article No.e18370, 2020. https://doi.org/10.2196/18370
- [8] L. Breiman, “Random forests,” Machine Learning, Vol.45, No.1, pp. 5-32, 2001. https://doi.org/10.1023/A:1010933404324
- [9] B. Widrow and M. E. Hoff, “Adaptive switching circuits,” IRE WESCON Convention Record, Vol.4, pp. 96-104, 1960.
- [10] C. J. C. H. Watkins and P. Dayan, “Q-learning,” Machine Learning, Vol.8, pp. 279-292, 1992. https://doi.org/10.1007/BF00992698
- [11] R. Timofeev, “Classification and regression trees (CART) theory and applications,” Master’s thesis, Humboldt University, 2004.
- [12] M. Christ, N. Braun, J. Neuffer, and A. W. Kempa-Liehr, “Time series feature extraction on basis of scalable hypothesis tests (tsfresh–a python package),” Neurocomputing, Vol.307, pp. 72-77, 2018. https://doi.org/10.1016/j.neucom.2018.03.067
- [13] A. Rechtschaffen and A. Kales, “A Manual of Standardized Terminology, Techniques and Scoring System for Sleep Stages of Human Subjects,” BIS/BRI University of California, 1968.
- [14] J. Cohen, “A coefficient of agreement for nominal scales,” Educational and Psychological Measurement, Vol.20, No.1, pp. 37-46, 1960. https://doi.org/10.1177/001316446002000104
 This article is published under a Creative Commons Attribution-NoDerivatives 4.0 Internationa License.
This article is published under a Creative Commons Attribution-NoDerivatives 4.0 Internationa License.