Paper:
Development of Ankle Support Shoes with Elastomer-Embedded Flexible Joints
Takehito Kikuchi*1, Taiki Oshimoto*2, Isao Abe*1, Kenichiro Tanaka*3, Yasue Asaumi*3, and Naoki Chijiwa*4
*1Faculty of Science and Technology, Oita University
700 Dannoharu, Oita 870-1192, Japan
*2Graduate School of Engineering, Oita University
700 Dannoharu, Oita 870-1192, Japan
*3Faculty of Welfare and Health Sciences, Oita University
700 Dannoharu, Oita 870-1192, Japan
*4Arizono Orthopedic Supplies Co., Ltd.
1-7-5 Higashida, Yahatahigashi-ku, Kitakyusyu, Fukuoka 805-8538, Japan
Walking is one of the most important activities in daily living, and difficulty walking presents a severe limitation. In this study, we develop shoes with elastomer-embedded flexible joints (EEFJ) that assist the tibialis anterior in its function during the initial stance and swing phase of the gait cycle. The EEFJ designed is suitable for shoes, with an adjustment mechanism incorporated for easy adjustment. To assess the ease of wearing, we measured the time it took four elderly subjects to wear the shoes for the first time. The donning time was less than one minute for all four participants. Furthermore, no one indicated discomfort when they walked naturally with the shoes. The supporting effect of the EEFJ shoes was assessed for ten healthy male subjects walking with their ankles relaxed. Statistical analysis reveals significant differences in the ankle at initial contact (p=0.02) and maximum plantar flexion (p=0.03). The average angle at initial contact while wearing the EEFJ shoes is 5.3° less than without it, and the average maximum plantar flexion is 5.1° less than without the shoes.
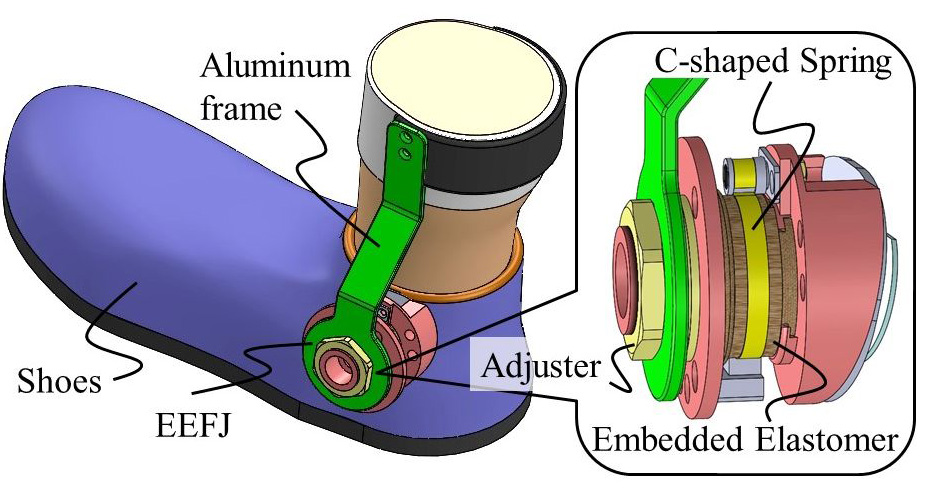
Developed shoes with elastomer-embedded flexible joints (EEFJ)
- [1] X. Chen, G. Mao, and S. X. Leng, “Frailty syndrome: an overview,” Clinical Interventions in Aging, Vol.9, pp. 433-441, 2014.
- [2] L. P. Fried, C. Tangen, J. Walston et al., “Frailty in Older Adults: Evidence for a Phenotype,” The J. of Gerontology Series A, Vol.56, Issue 3, pp. M146-M157, 2001.
- [3] M.-V. Castell, M. Sanchez, R. Julian, R. Queipo, S. Martin, and A. Otero, “Frailty prevalence and slow walking speed in persons age 65 and older: implications for primary care,” BMC Family Practice, Vol.14, No.86, 2013.
- [4] V. Inman, H. Ralston, and F. Todd, “Human walking,” Williams & Wilkins, 1981.
- [5] J. Lexell, C. C. Taylor, and M. Sjostrom, “What is the cause of the ageing atrophy? Total number, size and proportion of different fiber types studieed in whole vastus lateralis muscle from 15- to 83-year-old men,” J. of the Neurological Sciences, Vol.84, pp. 275-294, 1988.
- [6] T. Kikuchi, S. Tanida, T. Yasuda, and T. Fujikawa, “Automatic Adjustment of Initial Drop Speed of Foot for Intelligently Controllable Ankle Foot Orthosis,” Proc. of 2013 IEEE/SICE Int. Symp. on System Integration, pp. 276-281, 2013.
- [7] T. Kikuchi, S. Tanida, K. Otsuki, T. Yasuda, and J. Furusho, “A Novel Estimating Method of the Gait State and Velocity Control in the Initial Stance Phase for the Intelligent Ankle Foot Orthosis with Compact MR Fluid Brake (i-AFO),” J. of the Japanese Society for Experimental Mechanics, Vol.10, pp. 240-246, 2010.
- [8] M. L. J. Atrs, R. Waaijiman, M. de Haart, R. Keukenkamp, F. Nollet, and S. A. Bus, “Offloading effect of therapeutic footwear in patients with diabetic neuropathy at high risk for plantar foot ulceration,” Diabetic Medicine, Vol.29, No.12, pp. 1534-1541, 2012.
- [9] N. A. Guidemond, P. Leffers, N. C. Schaper, A. P. Sanders, F. Nieman, P. Willems, and G. H. I. M. Walenkamp, “The effects of insole configurations on forefoot plantar pressure and walking convenience in diabetic patients with neuropathic feet,” Clinical Biomechanics, Vol.22, Issue 1, pp. 81-87, 2007.
- [10] J. B. Redford, “Orthoses,” J. V. Basmajian and R. L. Kirby (Eds.), “Medical Rehabilitation,” Williams & Wilkins, 1984.
- [11] T. Kikuchi, K. Ishiya, I. Abe, S. Tanida, and T. Yasuda, “Novel ankle orthosis with elastomer-embedded flexible joint,” Proc. of 2017 Int. Conf. on Rehabilitation Robotics (ICORR), pp. 1124-1129, 2017.
- [12] I. Abe, T. Kikuchi, R. Kai, and S. Tanida, “Ankle supporter with elastomer-embedded flexible joint,” Proc. of 2016 IEEE/SICE Int. Symp. on System Integration (SII), pp. 126-131, 2016.
- [13] T. Oshimoto, I. Abe, T. Kikuchi, N. Chijiwa, T. Yabuta, K. Tanaka, and Y. Asaumi, “Gait Measurement for Walking Support Shoes with Elastomer-Embedded Flexible Joint,” Proc. of 2019 IEEE/SICE Int. Symp. on System Integrations (SII), pp. 537-542, 2019.
- [14] S. J. Lee and J. Hidler, “Biomechanics of overground vs. treadmill walking in healthy individuals,” J. of Applied Physiology, Vol.104, No.3, pp. 747-755, 2006.
- [15] R. W. Bohannon, “Reference values for extremity muscle strength obtained by hand-held dynamometry from adults aged 20 to 79 years,” Archives of physical medicine and rehabilitation, Vol.78, No.1, pp. 26-32, 1997.
- [16] J. Perry and J. Burnfield, “Gait analysis: normal and pathological function,” Slack Inc., pp. 55-56, 2010.
- [17] R. E. Isman and V. T. Inman, “Anthropometric studies of the human foot and ankle,” Bulletin of prosthetics research, Vols.10-11, pp. 97-129, 1969.
 This article is published under a Creative Commons Attribution-NoDerivatives 4.0 Internationa License.
This article is published under a Creative Commons Attribution-NoDerivatives 4.0 Internationa License.